
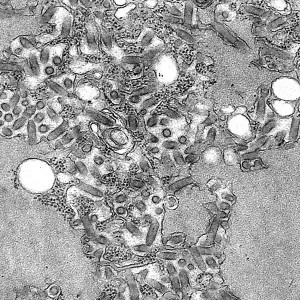
So What Is Rabies?
In a word, it is a virus, just like the common cold. The difference is that it affects not the respiratory system, but the central nervous system and brain. Moreover, unlike most viruses (many of which are species-specific), this virus can infect all warm-blooded species of animals, primarily mammals, including dogs, cats, and people. For most infected animals (humans included), once symptoms appear, the mortality rate is virtually 100%. Out of the tens of thousands of deaths worldwide from rabies every year, fewer than ten people are known to have survived. Fortunately, few of these deaths occur in the United States, thanks to a concerted effort, across all states, to limit if not eradicate this scourge.
The medical literature of the ancient world abounds with purported remedies for rabies, which was recognized as a particularly insidious disease at least 3,000 years ago. None of those remedies ever cured a thing, until Louis Pasteur developed an effective vaccine in 1885.
How Rabies Is Spread
Because it is present in the saliva of infected animals, the virus is typically transmitted by bite, or when the saliva of an infected animal enters an open wound or mucous membrane (in the eyes, nose, or mouth). In the United States, widespread immunization of livestock and pets has largely diminished that avenue of transmission to humans.
The bigger risk comes from the bite of wild animals infected with the disease, most commonly bats, raccoons, foxes, coyotes, and skunks. Some mammals, such as hamsters, squirrels, chipmunks, rats, mice, and other rodents, almost never contract rabies (if a rabid animal attacks them, they are usually killed before they can develop the disease). Birds, lizards, amphibians, and fish can neither carry nor naturally contract rabies.
Symptoms of Rabies
Once infected, humans may not show symptoms until one to three months after infection (though that incubation period can vary from one week to a year). It all depends on the severity and location of the contaminated wound. The virus first replicates within the muscle cells close to the site of infection, and does so without stimulating the host’s immune system. After that, it travels along neural pathways to the spinal cord, working its way up from there toward the brain.
At first, fever and headache are not uncommon. As the disease progresses, it eventually attacks the central nervous system and finally the brain, causing symptoms such as paralysis, anxiety, paranoia, hallucinations, and ultimately coma and death. One of the most striking symptoms is hydrophobia (“fear of water”), a term once commonly used to refer to rabies, since in the later stages of the disease the infected person may have difficulty swallowing and so exhibits an aversion to drinking water.
In animals, symptoms typically present as a noticeable change in normal behavior. Feral animals may seem unusually docile or fearless around people, or pets may become unaccountably aggressive toward their owners. Other symptoms include irritability, unprovoked growling, staggering, disorientation, muscle spasms, and generally erratic movements and activity. In the final stage of the disease, paralysis of the jaw and throat muscles will cause an inability to swallow, leading to drooling and foaming at the mouth. Death follows soon after.
Treatment and Prevention of Rabies
Once the initial incubation period has ended and symptoms begin to appear in a person, there is no effective cure for rabies; for all practical purposes, it is invariably fatal. For that reason, if an individual suspects they may have been exposed to the rabies virus (by coming in contact with the saliva of a potentially infected animal), urgent steps must be taken. If possible, capture the animal for diagnostic testing in a lab to determine whether it is in fact carrying the disease. For future reference, here is a short video on a safe and simple procedure for capturing a bat that may have found its way into your home—a not uncommon occurrence!
Prompt treatment after exposure can help prevent rabies infection. If you have suffered a wound from an animal bite or scratch, wash it immediately and thoroughly with soap and water, and then seek medical attention. Your doctor, in consultation with state and/or local health authorities, will decide whether a rabies vaccine regimen (post-exposure prophylaxis, or PEP) is warranted.
For domestic dogs and cats, the best treatment by far is—prevention!
Protect Your Pets with Rabies Tags
Of course, by itself a rabies tag does not prevent or offer protection against the disease. Rather, it signifies that your pet has been properly vaccinated as required by local statute, and that the pet owner is keeping those shots up to date.
It can even indicate what year the vaccination took place. Most rabies tags issued by authorized vets or county jurisdictions follow the standards of accepted veterinary practice by using a different shape every year, per the suggested protocol set forth by the National Association of State Public Health Veterinarians (NASPHV). For example, the 2016 rabies tag was heart-shaped; the 2017 rabies tag is a rosette, or flower shape; and the recommended shape for 2018 is an oval/teardrop. NOTE: Now available at Ketchum Mfg. Co. are 2019 rabies tags (which are bell-shaped).

(blue rosette)

(green bell)
Besides serving as a reminder to pet owners to keep their animal’s shots up to date, this rabies tag-shape protocol has another benefit in preventing a tragic mistake. If your pet gets lost, an animal control officer can tell at a glance what year the dog or cat was last vaccinated, and determine from that whether or not it poses a disease risk to anyone handling it. For that reason, you should never keep a “collection” of rabies tags on your pet’s collar. There should only be one at a time. As soon your pet gets re-vaccinated, remove the old rabies tag and replace it with the new one.
Finally, take no chances even if your dog or cat has been vaccinated. Keep the family pet indoors at night, and don’t leave it unattended when it goes outside. If you believe it has come in contact with or been bitten by a possibly rabid animal, immediately contact your vet for treatment. Any bite requires medical care, of course. But a booster shot may also be needed to strengthen your pet’s immunity to the disease.
For additional information, please see the national Centers for Disease Control and Prevention (CDC) rabies page.
Current Ketchum Mfg. Co. Rabies Tags
Available at our website…









